Nuclear Metabolic Fingerprints: How Hidden Enzymes on DNA Could Transform Cancer Treatment
A groundbreaking study published in Nature Communications has revealed a hidden metabolic network operating directly on human DNA within the cell nucleus. Researchers discovered over 200 metabolic enzymes attached to chromatin, forming unique 'nuclear metabolic fingerprints' that vary between tissues and cancer types. This unexpected link between metabolism and gene regulation challenges long-held biological assumptions and offers profound implications for understanding tumor development, treatment resistance, and personalized cancer therapies.
For decades, cell biology textbooks have presented a clear division of labor: the nucleus houses and regulates our genetic blueprint, while metabolic enzymes operate in the cytoplasm and mitochondria to produce energy and cellular building blocks. A revolutionary discovery is shattering this fundamental paradigm. Researchers from the Center for Genomic Regulation have uncovered a hidden metabolic network operating directly on human DNA inside the cell nucleus, revealing unexpected connections that could reshape our understanding of cancer biology and treatment.

The Discovery of Nuclear Metabolic Enzymes
Using advanced techniques to isolate proteins physically attached to chromatin—the complex of DNA and proteins that packages genetic material—scientists made a startling observation. More than 200 metabolic enzymes, typically associated with energy production in other cellular compartments, were found directly bound to human DNA within the nucleus. This represents approximately 7% of all chromatin-associated proteins, suggesting what researchers describe as a 'mini metabolism' operating within the nuclear environment.
The research team examined 44 cancer cell lines and 10 healthy cell types from different tissues, discovering that each cell type displays a distinctive arrangement of these nuclear metabolic enzymes. These unique patterns form what scientists have termed a "nuclear metabolic fingerprint," marking the first evidence that human cells carry such specific nuclear signatures that vary between tissues and disease states.

Tissue-Specific Patterns and Cancer Implications
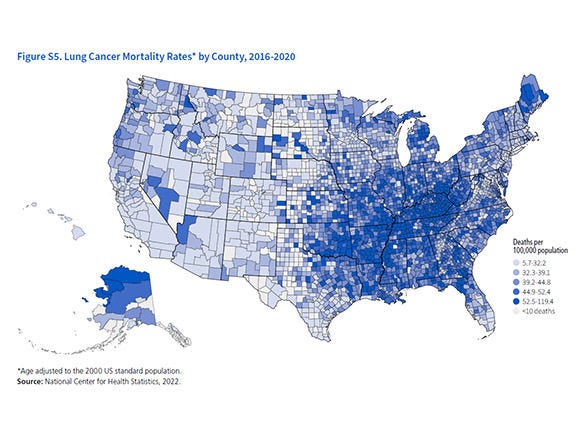
The study revealed striking differences in nuclear metabolism between cancer types. Breast cancer cells showed significantly higher nuclear levels of oxidative phosphorylation enzymes—proteins responsible for generating cellular energy—compared to lung cancer cells. When researchers examined actual tumor samples from patients, they confirmed these tissue-specific patterns, suggesting that nuclear metabolic fingerprints could serve as biomarkers for cancer diagnosis and classification.
"We've been treating metabolism and genome regulation as two separate universes, but our work suggests they're talking to each other, and cancer cells might be exploiting these conversations to survive," explains Dr. Savvas Kourtis, first author of the study published in Nature Communications. This connection may help explain why tumors originating from different tissues, even when carrying identical genetic mutations, often respond very differently to chemotherapy, radiation, or targeted therapies.
Functional Roles in DNA Repair and Genome Stability
Beyond mere presence, researchers investigated what these nuclear enzymes actually do. Experiments revealed that specific metabolic enzymes gather near chromatin when DNA damage occurs, suggesting they play active roles in genome repair. One enzyme in particular, IMPDH2, demonstrated location-dependent functionality: when confined to the nucleus, it helped maintain genome stability, while the same enzyme restricted to the cytoplasm influenced entirely different cellular pathways.
This discovery has profound implications for cancer treatment. Many therapies work by inducing DNA damage in rapidly dividing cancer cells, while others target metabolic processes. The newly discovered link between nuclear metabolism and DNA repair suggests these two therapeutic approaches may be more interconnected than previously understood. "Many of these enzymes synthesize essential building blocks of life, and their nuclear localization is associated with DNA repair. Their presence in the nucleus may therefore directly shape how cancer cells respond to genotoxic stress, a hallmark of many chemotherapeutic treatments," says Dr. Sara Sdelci, corresponding author of the study.
Unanswered Questions and Future Directions
Despite these groundbreaking findings, significant mysteries remain. Researchers still need to determine whether all nuclear metabolic enzymes are active in their chromatin-bound state and what specific biochemical reactions they catalyze. "Each enzyme may have its own, unique nuclear function, so this must be addressed one by one," notes Dr. Kourtis. Additionally, scientists are puzzled by how these large enzymes enter the nucleus through nuclear pores that theoretically should exclude molecules of their size, suggesting unknown transport mechanisms.
The discovery opens entirely new avenues for cancer research and treatment development. Mapping nuclear metabolic fingerprints across different cancers could lead to more precise diagnostic tools and reveal novel therapeutic targets. By understanding how cancer cells exploit nuclear metabolism for survival and adaptation, researchers may develop strategies to disrupt these processes specifically in malignant cells while sparing healthy tissue.
Conclusion: A New Frontier in Cellular Biology
The revelation of nuclear metabolic fingerprints represents a paradigm shift in our understanding of cellular organization and function. What was once considered separate biological systems—metabolism and gene regulation—now appears intricately connected through a network of enzymes operating directly on our genetic material. This discovery not only advances fundamental biological knowledge but also offers promising translational potential for improving cancer diagnosis, treatment selection, and therapeutic development.
As research continues to unravel the complexities of nuclear metabolism, we stand at the threshold of a new era in molecular medicine—one where the hidden conversations between metabolism and genetics may hold the key to more effective, personalized approaches to combating cancer and other diseases.