How Gut-Brain Signaling Failure Drives Age-Related Memory Loss
Groundbreaking research reveals that age-related cognitive decline may be driven by intestinal interoceptive dysfunction, where impaired gut-brain communication leads to memory loss. A new study published in Nature identifies a specific pathway involving gut bacteria, inflammatory responses, and vagal nerve signaling that contributes to hippocampal dysfunction during aging. The research demonstrates that age-associated microbiome changes, particularly the outgrowth of Parabacteroides goldsteinii, produce metabolites that trigger peripheral inflammation, impair vagal signaling, and reduce hippocampal neuronal activation. These findings suggest that targeting gut-brain communication pathways could offer new therapeutic approaches for age-related cognitive decline.
Age-related cognitive decline represents one of the most significant challenges to healthy aging, affecting millions worldwide with no effective treatments currently available. While brain-intrinsic factors have long been the focus of research, emerging evidence points to brain-extrinsic influences, particularly from the gastrointestinal system. A groundbreaking study published in Nature reveals that intestinal interoceptive dysfunction—the impaired communication between gut and brain—plays a crucial role in driving age-associated memory loss. This research provides compelling evidence that the gut microbiome influences cognitive aging through a specific pathway involving bacterial metabolites, peripheral inflammation, and vagal nerve signaling.
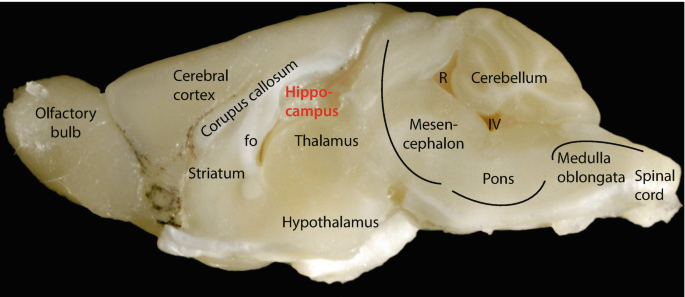
The Gut-Brain Connection in Cognitive Aging
The gastrointestinal microbiome has emerged as a critical regulator of brain function and cognitive processes. Recent research demonstrates that gut microbial communities change significantly with age, and these alterations can influence brain health through various signaling pathways. The study from Nature reveals that the aging microbiome produces specific metabolites that interfere with normal gut-brain communication, ultimately leading to impaired memory formation and recall. This represents a paradigm shift in understanding cognitive aging, suggesting that peripheral interventions targeting the gut may offer new approaches to preserving brain function.
Interoception—the sense of the internal state of the body—relies on continuous communication between peripheral organs and the brain through neural and humoral pathways. The vagus nerve serves as a major conduit for this communication, transmitting signals from the gut to brain regions involved in memory processing, particularly the hippocampus. When this interoceptive signaling becomes impaired, as occurs during aging, the brain receives diminished input about the body's state, potentially contributing to cognitive decline. The research demonstrates that this impairment is not merely a passive consequence of aging but can be actively influenced by specific microbiome changes.

The Microbial Pathway to Memory Impairment
The research identifies a specific bacterial species, Parabacteroides goldsteinii, whose abundance increases with age and contributes significantly to cognitive decline. Through a series of elegant experiments using mouse models, researchers demonstrated that transferring gut microbiota from aged mice to young recipients accelerated cognitive aging in the young animals. This effect was specific to microbial transfer and not due to social factors, as confirmed by germ-free experiments where co-housing with aged animals without microbial transfer did not impair cognition.
P. goldsteinii produces medium-chain fatty acids (MCFAs), particularly 3-hydroxyoctanoic acid, which accumulate in the intestinal lumen during aging. These metabolites trigger a cascade of events that ultimately impair hippocampal function. The study shows that oral administration of these MCFAs alone is sufficient to recapitulate the cognitive deficits observed in aged animals, confirming their role as key mediators in the pathway from microbiome changes to brain dysfunction.
From Gut Metabolites to Brain Inflammation
The mechanism by which MCFAs impair cognition involves activation of the GPR84 receptor on peripheral myeloid cells. GPR84 signaling triggers the production of pro-inflammatory cytokines, including tumor necrosis factor (TNF) and interleukin-1β (IL-1β), particularly in adipose tissue surrounding the gastrointestinal tract. This localized inflammation then impairs the function of vagal afferent neurons that normally transmit gut signals to the brain.
Remarkably, this inflammatory process occurs peripherally without requiring central nervous system involvement. The research demonstrates that peripheral myeloid cell activation is sufficient to disrupt vagal signaling and hippocampal function, even when brain inflammation is minimal. This finding challenges traditional views that cognitive decline requires direct brain inflammation and suggests that peripheral interventions targeting gut-associated inflammation could protect brain function.
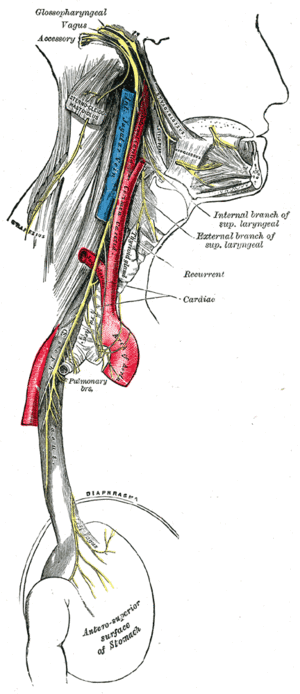
Vagal Signaling and Hippocampal Function
The vagus nerve serves as the critical link between peripheral inflammation and hippocampal dysfunction. Research shows that MCFA-induced inflammation specifically impairs the activation of vagal neurons in response to intestinal stimuli. Using advanced calcium imaging techniques, scientists demonstrated that nutrient infusion into the intestine triggered significantly weaker responses in vagal neurons from animals with age-associated microbiome changes compared to young controls.
This impaired vagal signaling leads to reduced neuronal activation in the hippocampus, particularly in response to novel experiences. The study shows that immediate-early gene expression—a marker of neuronal activation—is blunted in the hippocampus of animals with age-associated microbiome changes. This reduced hippocampal responsiveness correlates directly with impaired performance in memory tasks, including novel object recognition and spatial learning tests.
Restoring Cognitive Function Through Intervention
The research identifies several potential intervention points along the gut-brain pathway that can restore cognitive function. Vagal nerve stimulation, either through chemogenetic activation or pharmacological means using low-dose capsaicin, completely reversed cognitive deficits in aged animals and young animals with age-associated microbiomes. Similarly, administration of gut peptides like cholecystokinin (CCK) and glucagon-like peptide-1 (GLP-1), which normally stimulate vagal signaling, restored hippocampal function and memory performance.
Targeting the inflammatory component also proved effective. Inhibition of GPR84 signaling using specific antagonists protected against MCFA-induced cognitive impairment. Depletion of peripheral myeloid cells using various approaches restored vagal function and hippocampal responses. Even more remarkably, treatment with bacteriophages targeting related bacterial species reduced intestinal MCFA levels and improved cognition in aged animals, suggesting microbiome modulation as a viable therapeutic strategy.

Implications for Human Cognitive Health
While this research was conducted in mouse models, the findings have significant implications for understanding and potentially treating age-related cognitive decline in humans. The pathway identified—from specific gut bacteria to metabolites, peripheral inflammation, vagal impairment, and hippocampal dysfunction—represents a novel framework for understanding the heterogeneity of cognitive aging. Individuals with different microbiome compositions or inflammatory profiles may experience different rates of cognitive decline based on this pathway's activity.
The concept of "interoceptomimetics"—compounds that stimulate gut-brain communication—emerges as a promising therapeutic approach. By enhancing vagal signaling or reducing peripheral inflammation, such interventions could potentially slow or reverse age-related cognitive decline without directly targeting the brain. This peripheral approach offers advantages in terms of safety and accessibility compared to central nervous system-targeted therapies.
Future Directions and Clinical Translation
Several important questions remain for future research. The precise polysynaptic pathway connecting vagal signaling to hippocampal function needs further elucidation, as does the mechanism by which chronic peripheral inflammation alters vagal excitability. The specific types and locations of peripheral myeloid cells involved in interoceptive dysfunction require identification. Most importantly, research must determine whether elements of this pathway contribute to cognitive decline in humans and whether interventions targeting this pathway prove effective in clinical settings.
Preliminary evidence suggests relevance to human health. Vagus nerve stimulation has shown promise in enhancing recognition memory and cognitive performance in human studies, though its application specifically for age-related decline requires investigation. The growing understanding of how diet, antibiotics, probiotics, and other microbiome-modulating interventions affect cognitive function in humans may provide indirect support for the pathway's relevance.
Conclusion
The discovery that intestinal interoceptive dysfunction drives age-associated cognitive decline represents a significant advance in understanding brain aging. By identifying a specific pathway from gut microbiome changes to hippocampal dysfunction, this research opens new avenues for intervention that target peripheral rather than central processes. The findings emphasize the importance of body-derived signals in maintaining cognitive function and highlight the potential of interoceptomimetics as a novel class of therapeutics for age-related memory loss. As research progresses, targeting gut-brain communication may emerge as a powerful strategy for promoting healthy cognitive aging and improving quality of life for older adults worldwide.