Brain Wave Biomarker Identified for Tracking Anaesthesia-Induced Unconsciousness
Scientists have discovered a distinctive brain-wave pattern that signals the transition into unconsciousness under general anaesthesia. The research, focusing on the widely used drug propofol, identified a faltering in the communication between key brain regions like the parietal cortex and thalamus as consciousness fades. This potential biomarker could help anaesthesiologists fine-tune drug dosing to avoid the risks of over- or under-sedation during surgery, moving beyond behavioral observation to a quantifiable biological measure of unconsciousness.
For decades, anaesthesiologists have relied on observable patient responses—like the loss of eyelid reflex or changes in breathing—to gauge when a patient has slipped into unconsciousness. This critical moment in surgery has lacked a precise, biological signature. Now, a new study published in Cell Reports Medicine offers a potential breakthrough: a distinctive brain-wave pattern that marks the slide into unconsciousness induced by the anaesthetic propofol. This discovery could pave the way for more precise and safer anaesthesia administration in operating rooms worldwide.

The Search for a Non-Behavioral Marker
The fundamental challenge in anaesthesiology has been the absence of a reliable, objective biomarker for consciousness. As noted in the Nature report on the research, scientists have long sought non-behavioral correlates. A quantifiable biological measure would allow doctors to move beyond guesswork and behavioral cues, enabling them to fine-tune drug dosing with unprecedented accuracy. The complications of over-sedation—such as prolonged recovery times and cardiovascular issues—and the dangers of under-sedation, including intraoperative awareness, highlight the urgent need for such a tool.
How the Brain Wave Biomarker Was Discovered
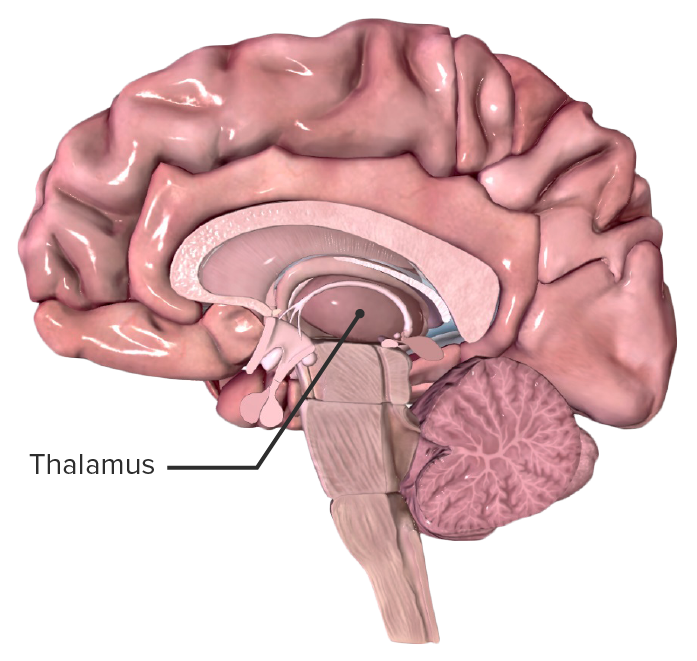
The research team, led by neuroscientists at Shanghai Jiao Tong University, studied 31 patients receiving propofol before surgery. Using a high-density array of 128 electrodes on each participant's scalp, they recorded the brain's electrical activity. Advanced mathematical techniques were then employed to infer signals originating from nine specific brain regions previously linked to consciousness, including the parietal cortex, occipital cortex, and the deeper thalamus.
The Key Finding: A Breakdown in Communication
The critical discovery was a change in the synchronization of alpha-band brain waves. In the awake state, these waves were highly synchronized between the parietal cortex and the thalamus, indicating robust communication between these areas. As propofol took effect and unconsciousness ensued, this synchronized interplay faltered. The connectivity between the parietal and occipital areas also showed significant changes. This breakdown in coordinated activity across key brain networks appears to be a hallmark of the loss of consciousness.
Implications for the Future of Anaesthesia
If validated by further research, this brain-wave pattern could serve as a translatable biomarker. Co-author Ti-Fei Yuan suggests this provides a concrete possibility for clinical application. In practice, monitoring this signature in real-time could give anaesthesiologists a direct window into a patient's brain state, allowing for dynamic adjustment of anaesthetic levels. This would represent a major shift from a one-size-fits-all dosing model to personalized, brain-state-guided anaesthesia.
However, the authors acknowledge limitations. The study focused solely on propofol, and the technique for inferring deep-brain signals from scalp recordings is still emerging. Future research must confirm if similar or distinct biomarkers exist for other anaesthetic agents.
Conclusion
The identification of a potential brain-wave biomarker for unconsciousness marks a significant step forward in neuroscience and clinical medicine. By providing an objective measure of a patient's state under anaesthesia, this research holds the promise of enhancing surgical safety, improving patient outcomes, and reducing anaesthesia-related complications. As this science translates from the lab to the operating room, it may fundamentally change how we monitor and manage the delicate state of unconsciousness.





